Breast cancer remains a critical women’s health challenge, but 2026 has delivered transformative advances that renew hope for patients worldwide. New treatments like antibody-drug conjugates, the oral SERD giredestrant, and the PIK3CA inhibitor zovegalisib are expanding options, particularly for those with metastatic disease. Immunotherapy has achieved a landmark 70% five-year survival rate for certain subtypes, a dramatic leap from previous years.
These breakthroughs gain deeper significance through Peta Murphy’s enduring legacy: a $1.5 million federal data registry that will finally make metastatic breast cancer patients visible in national health statistics. Developed by AIHW and BCNA, this registry ensures that advances in women’s health reach every Australian who needs them. Explore the latest women’s health resources for more context.
- 2026 breakthroughs include antibody-drug conjugates, oral SERDs (giredestrant), and PIK3CA inhibitors (zovegalisib) offering new targeted options.
- Immunotherapy advances have achieved a 70% five-year survival rate for certain breast cancers.
- Peta Murphy’s $1.5M federal funding established a national metastatic breast cancer data registry to track stage and recurrence, addressing patient invisibility.
What Are the Latest Breast Cancer Advances in 2026?
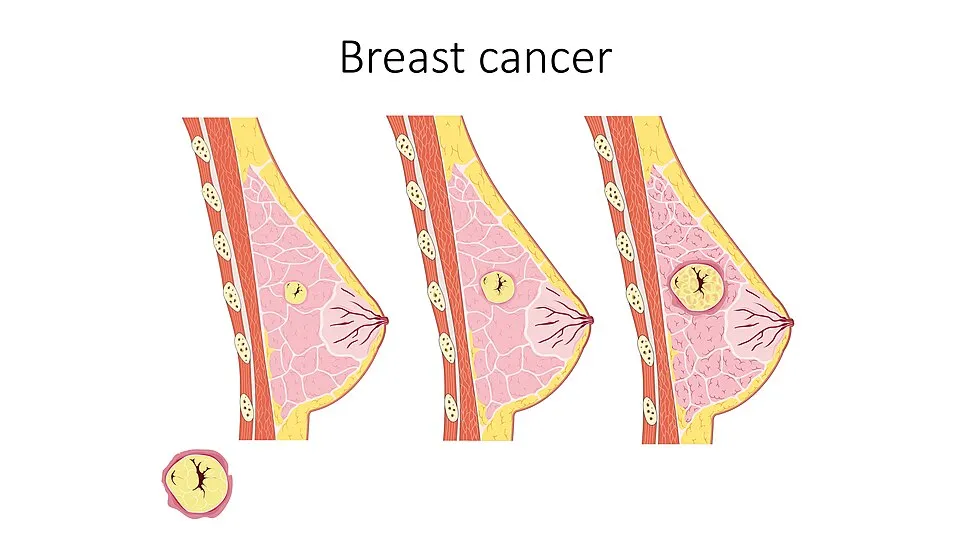
The landscape of breast cancer treatment is evolving rapidly, with 2026 marking a year of significant regulatory approvals and clinical breakthroughs. These innovations focus on precision targeting, improved survival, and enhanced quality of life for patients across all stages.
Giredestrant: Oral SERD That Reduces Distant Recurrence Risk
Giredestrant is an oral selective estrogen receptor degrader (SERD) that represents a major advancement for hormone receptor-positive (HR+) breast cancer, which accounts for about 70% of all cases. Unlike older injectable SERDs such as fulvestrant, giredestrant’s oral formulation offers unparalleled convenience, eliminating the need for frequent clinic visits and improving long-term adherence. The Breast Cancer Research Foundation (BCRF) reported in January 2026 that giredestrant significantly reduces the risk of distant recurrence—the spread of cancer to organs like bone, liver, or brain—in HR+ patients.
This finding comes from pivotal Phase III trials that compared giredestrant to standard endocrine therapy, showing a clear improvement in disease-free survival. For patients, this means a lower chance of cancer returning in a life-threatening form, all while taking a daily pill at home. The drug’s development reflects the broader shift toward patient-centric cancer care, where efficacy is matched by ease of use.
As giredestrant moves through regulatory review in 2026, it promises to become a new standard of care, particularly for those who cannot tolerate injections or who live in remote areas. Its success also underscores the importance of continued investment in endocrine therapy research, a cornerstone of HR+ breast cancer management. For those seeking women’s health information, giredestrant exemplifies how far treatment has come.
Zovegalisib’s FDA Breakthrough: Targeting PIK3CA-Mutated Metastatic Breast Cancer
For the subset of metastatic breast cancer patients with a PIK3CA mutation, 2026 brings a beacon of hope in the form of zovegalisib. This targeted therapy has rapidly ascended through the regulatory pipeline, offering a much-needed option after earlier treatments fail.
- Zovegalisib (RLY-2608) is a potent, selective PIK3CA inhibitor developed by Rhizen Pharmaceuticals. It is designed to be combined with fulvestrant, blocking the PI3K pathway that drives cancer growth in mutated cells.
- FDA breakthrough therapy designation was granted in February/March 2026 based on compelling Phase II data. The designation accelerates development and review, reflecting the drug’s potential to address an unmet medical need.
- Approximately 40% of HR+ breast cancers harbor PIK3CA mutations, according to Susan G. Komen’s 2026 data. This means a large patient population could benefit from zovegalisib, especially those who have progressed after CDK4/6 inhibitor therapy.
- Significance: Zovegalisib provides a new line of defense for metastatic patients whose cancer has become resistant to first-line targeted therapies. Its mechanism specifically attacks the genetic driver, offering a more precise and potentially less toxic alternative to chemotherapy.
The approval process for zovegalisib highlights how 2026 is bridging global innovations with local patient needs. Australian clinicians and advocates are closely watching this development, hoping it will soon be accessible through the PBS. Learn more about cancer screening programs that can identify high-risk patients early.
Targeted Therapy Landscape: Comparing 2026’s Leading Advances
| Therapy Class | Example Drug | Mechanism | Target Patient Group | Key Benefit | Development Status |
|---|---|---|---|---|---|
| SERD | Giredestrant | Oral selective estrogen receptor degrader | HR+ breast cancer (early and metastatic) | Reduces distant recurrence risk; oral convenience | Clinical use in 2026 (BCRF report Jan 2026) |
| PIK3CA inhibitor | Zovegalisib (RLY-2608) | Inhibits mutated PIK3CA protein | HR+/HER2- mBC with PIK3CA mutation post-CDK4/6i | New option after CDK4/6 inhibitor failure | FDA breakthrough designation (Mar 2026) |
These two therapies illustrate the power of personalized medicine. Giredestrant benefits a broad HR+ population, while zovegalisib is reserved for those with a specific genetic mutation, identified through molecular testing. Both represent a shift from one-size-fits-all chemotherapy to treatments that target the unique biology of each tumor.
This precision approach improves efficacy and reduces unnecessary side effects. However, access remains a challenge: targeted therapies often come with high price tags, requiring robust evidence of cost-effectiveness to secure PBS listing. Australia’s new metastatic breast cancer data registry will provide that evidence by tracking real-world outcomes.
The landscape is also expanding to include antibody-drug conjugates (ADCs), which deliver chemotherapy directly to cancer cells, and next-generation oral SERDs. As these therapies move through clinical trials, the line between early-stage and metastatic treatment continues to blur, offering longer, healthier lives for patients. For insights into Medicare health policies that determine coverage, stay informed through advocacy groups like BCNA.
The $1.5M Metastatic Breast Cancer Data Registry: Peta Murphy’s Policy Legacy

Peta Murphy’s fight for metastatic breast cancer patients has crystallized into a concrete policy achievement: a national data registry that will transform how Australia understands and treats advanced disease. This initiative addresses a decades-long invisibility that left thousands of patients uncounted and under-served.
The Invisibility of Metastatic Breast Cancer: BCNA’s 2025 Report
Metastatic breast cancer (mBC) is stage IV disease that has spread beyond the breast to distant organs. It is incurable and requires lifelong treatment, yet for years, these patients have been statistically invisible. The Breast Cancer Network Australia (BCNA) report “From Invisibility to Influence,” released in November 2025, exposed how routine cancer registries fail to capture the full mBC population.
Most registries record stage at initial diagnosis but do not systematically track recurrences that occur months or years later. As a result, a patient diagnosed with early-stage disease who later develops metastasis may never be counted as an mBC case. This gap means the true prevalence and incidence of metastatic breast cancer in Australia are unknown.
The impact is profound: without accurate numbers, funding for research, support services, and specialized care remains inadequate. Clinical trials often exclude mBC patients, and pharmaceutical companies hesitate to invest in therapies for a population that cannot be quantified. Patients themselves report feeling overlooked, as if their disease is less legitimate than early-stage cancer.
BCNA’s report called for a national registry to end this erasure, and Peta Murphy championed that cause until her final days. Her advocacy was personal; she understood the mBC journey from her own experience. For a deeper look at Peta Murphy’s personal breast cancer journey, explore this dedicated archive.
$1.5M Federal Funding: Building a National Data Registry
The $1.5 million AUD commitment from the Albanese Government, announced in February 2024 and extending through 2026, provides the financial foundation for the registry. This funding was secured by Peta Murphy before her passing in December 2023, ensuring her vision would become reality. Key implementation details:
- Partners: The Australian Institute of Health and Welfare (AIHW) is developing the registry in close partnership with Breast Cancer Network Australia (BCNA), bringing together statistical expertise and patient advocacy.
- Data to be collected: The registry will capture stage at diagnosis, recurrence status, tumor biology (HR/HER2 status, genetic mutations), treatment sequences, and survival outcomes. It will include both de novo metastatic cases and those who recur after early-stage diagnosis.
- How it addresses gaps: By mandating reporting from all states and territories, the registry will create a complete national picture. It will also link with existing AIHW cancer data to avoid duplication and ensure longitudinal follow-up.
- Timeline: Development began in 2024; pilot data collection started in selected hospitals in 2025, with full national rollout expected in 2026. The first comprehensive report on mBC prevalence and outcomes is anticipated in late 2026 or early 2027.
- Expected impact: The registry will provide the evidence base for PBS submissions, clinical guideline updates, and service planning. It will also empower patients by giving them a voice in the data that shapes their care.
This initiative represents a major step toward equitable, data-driven cancer policy in Australia. It also highlights how social medicine in practice can address systemic gaps by centering patient experiences in health system design.
From Data to Policy: Enabling Access to Targeted Therapies
Before the registry: Policymakers lacked reliable Australian data on the metastatic breast cancer population. When pharmaceutical companies applied to list expensive targeted therapies on the PBS, the Pharmaceutical Benefits Advisory Committee (PBAC) often found the evidence insufficiently tailored to the local context. International studies might show benefit, but without knowing how many Australian patients would qualify or how the therapy would fit into existing treatment sequences, PBAC frequently rejected or deferred applications.
This left patients without access to drugs like zovegalisib or giredestrant, forcing them to rely on older, less effective treatments or to pay out-of-pocket. The data void also hindered advocacy; BCNA could not quantify the unmet need, making it harder to argue for funding.
After the registry: With accurate, real-world data, the landscape changes. The registry will show exactly how many Australian mBC patients have PIK3CA mutations, how many progress after CDK4/6 inhibitors, and how current treatments perform. This evidence will strengthen PBS applications, demonstrating the number of potential beneficiaries and the therapy’s value in the Australian setting.
It will also help identify disparities—such as rural vs. urban access—and guide policy to correct them. Peta Murphy’s legacy is that she turned an abstract problem—invisibility—into a solvable one by securing the funds for this registry.
Her foresight ensures that future policy decisions are grounded in Australian data, not guesswork. As 2026 breakthroughs arrive, the registry will be the conduit that translates scientific advances into tangible patient access, fulfilling Murphy’s belief that every patient deserves to be seen and served.
Immunotherapy and AI: 2026’s Survival and Detection Breakthroughs
While targeted therapies dominate headlines, immunotherapy and artificial intelligence are quietly revolutionizing breast cancer outcomes and detection. Together, they promise earlier diagnosis, more effective treatment, and longer survival.
70% Five-Year Survival: Immunotherapy’s 2026 Milestone
Immunotherapy has achieved a stunning 70% five-year survival rate for certain breast cancer patients, a figure that would have seemed impossible a decade ago. This milestone, reported by Cancer Research in February 2026, primarily applies to early-stage triple-negative breast cancer (TNBC), a historically aggressive subtype with limited treatment options. The improvement stems from the addition of checkpoint inhibitors—pembrolizumab (Keytruda) and atezolizumab (Tecentriq)—to standard chemotherapy.
Landmark trials such as KEYNOTE-355 and IMpassion031 demonstrated that combining immunotherapy with chemo before surgery significantly reduces the risk of recurrence. For TNBC patients, the five-year survival rate has jumped from around 40-50% with chemotherapy alone to 70% with the addition of immunotherapy. This represents a paradigm shift: TNBC is no longer a uniformly fatal diagnosis but a disease with a realistic chance of long-term remission.
The impact extends to the metastatic setting as well, where immunotherapy has improved progression-free survival. These results underscore the power of harnessing the immune system, a strategy that was once experimental but is now standard of care for many.
The 70% figure is a beacon of hope, showing how far we have come and how much further we can go with continued research and advocacy. Public health initiatives are critical to ensure these advances reach all populations, including underserved communities.
Liquid Biopsies: Detecting ctDNA and Minimal Residual Disease
Liquid biopsies—simple blood tests that analyze circulating tumor DNA (ctDNA)—are emerging as a transformative tool for monitoring breast cancer, especially after initial treatment. Their 2026 breakthrough status is reshaping follow-up care.
- What they are: A liquid biopsy draws blood and uses highly sensitive sequencing to detect fragments of DNA shed by tumor cells into the bloodstream. This provides a real-time snapshot of the cancer’s genetic makeup without needing a tissue biopsy.
- Minimal residual disease (MRD) detection: After surgery or radiation, ctDNA can identify microscopic amounts of cancer that remain, often months before imaging would show a recurrence. This early warning allows for timely intervention.
- Benefits: ctDNA monitoring guides treatment decisions—such as whether to add chemotherapy after surgery—tracks response to systemic therapy, and detects emerging resistance mutations. It is repeatable and non-invasive, making it ideal for longitudinal monitoring.
- Why it’s a breakthrough: Traditional imaging scans are expensive, infrequent, and may miss microscopic disease. Liquid biopsies offer a dynamic, molecular-level view that can be performed every few months, potentially catching recurrence when it is most treatable. FDA-cleared tests like Guardant360 and Signatera are now being integrated into clinical guidelines, with Australian oncology centers adopting them in 2026.
For patients navigating the post-treatment phase, liquid biopsies provide reassurance and actionable data. They also highlight the importance of ongoing surveillance, a topic covered in resources on patient support funds that help cover monitoring costs.
AI-Powered Diagnostics: Enhancing Screening Accuracy
Artificial intelligence is no longer a futuristic concept; it is actively improving breast cancer detection and diagnosis in 2026. AI algorithms, trained on vast datasets of mammograms and pathology slides, are being deployed across screening programs and diagnostic centers. In mammography, AI tools like ProFound AI and Koios DS have demonstrated the ability to increase cancer detection rates by 5-10% while reducing false positives by 20-30%.
This means fewer unnecessary callbacks and biopsies, alleviating patient anxiety and healthcare costs. AI acts as a second reader, highlighting subtle abnormalities that even experienced radiologists might miss, and can triage normal exams so that human experts focus on suspicious cases. In pathology, AI assists in grading tumors and identifying molecular subtypes from biopsy samples, accelerating turnaround times and ensuring consistency.
The technology is particularly valuable in regions with radiologist shortages, where AI can help maintain screening quality. Australian breast screening services are piloting AI in 2026, with early results showing improved efficiency and accuracy. As AI models continue to learn from global data, their performance will only improve.
However, challenges remain around data privacy, algorithm bias, and the need for human oversight. The integration of AI into routine care marks a significant step toward more precise, efficient, and accessible breast cancer diagnostics. These advances also intersect with social medicine by potentially reducing disparities in screening quality between urban and rural areas.
The most surprising finding is immunotherapy’s 70% five-year survival rate for triple-negative breast cancer—a leap that redefines prognosis for a once-feared subtype. To ensure all patients benefit from such advances, support comprehensive cancer data collection like the metastatic breast cancer registry, and discuss targeted therapy options with your oncologist if you are facing a breast cancer diagnosis. Peta Murphy’s legacy reminds us that data-driven advocacy turns scientific breakthroughs into real-world hope, especially in the realm of women’s health.
